ELIE DOLGIN
Clinicians at St. Michael’s Hospital in Toronto used the new imaging probe to evaluate narrowed brain arteries in a patient with atherosclerosis. ST. MICHAEL’S FOUNDATION
Neurosurgeon Vitor Mendes Pereira has grown accustomed to treating brain aneurysms with only blurry images for guidance.
OPTICAL COHERENCE TOMOGRAPHY
FIBER OPTICS
BRAIN IMAGING
Equipped with a rough picture of the labyrinthine network of arteries in the brain, he does his best to insert mesh stents or coils of platinum wire—interventions intended to promote clotting and to seal off a bulging blood vessel.
The results are not always perfect. Without a precise window into the arterial architecture at the aneurysm site, Pereira says that he and other neurovascular specialists occasionally misplace these implants, leaving patients at a heightened risk of stroke, clotting, inflammation, and life-threatening ruptures. But a new fiber-optic imaging probe offers hope for improved outcomes.
PEREIRA ET AL./SCIENCE TRANSLATIONAL MEDICINE
According to Pereira’s early clinical experience, the technology—a tiny snake-like device that winds its way through the intricate maze of brain arteries and, using spirals of light, captures high-resolution images from the inside-out—provides an unprecedented level of structural detail that enhances the ability of clinicians to troubleshoot implant placement and better manage disease complications.
“We can see a lot more information that was not accessible before,” says Pereira, director of endovascular research and innovation at St. Michael’s Hospital in Toronto. “This is, for us, an incredible step forward.”
And not just for brain aneurysms. In a report published today in Science Translational Medicine, Pereira and his colleagues describe their first-in-human experience using the platform to guide treatment for 32 people with strokes, artery hardening, and various other conditions arising from aberrant blood vessels in the brain.
Whereas before, with technologies such as CT scans, MRIs, ultrasounds, and x-rays, clinicians had a satellite-like view of the brain’s vascular network, now they have a Google Street View-like perspective, complete with in-depth views of artery walls, plaques, immune cell aggregates, implanted device positions, and more.
“The amount of detail you could get you would never ever see with any other imaging modality,” says Adnan Siddiqui, a neurosurgeon at the University at Buffalo, who was not involved in the research. “This technology holds promise to be able to really transform the way we evaluate success or failure of our procedures, as well as to diagnose complications before they occur.”
A Decade of Innovation
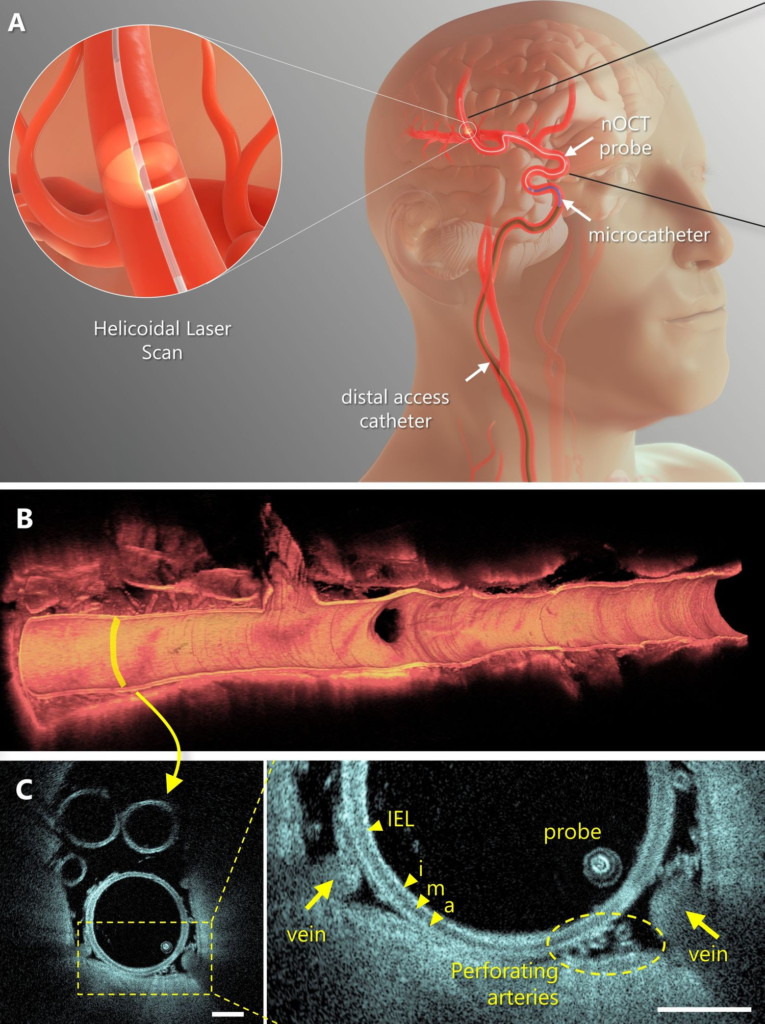
The new fiber-optic probe is flexible enough to snake through the body’s arteries and provide previously unavailable information to surgeons.PEREIRA ET AL./SCIENCE TRANSLATIONAL MEDICINE
The new imaging platform is the brainchild of Giovanni Ughi, a biomedical engineer at the University of Massachusetts’ Chan Medical School in Worcester. About a decade ago, he set out to adapt a technique called optical coherence tomography (OCT) for imaging inside the brain’s arteries.
OCT relies on the backscattering of near-infrared light to create cross-sectional images with micrometer-scale spatial resolution. Although OCT had long been used in clinical settings to generate pictures from the back of the eye and from inside the arteries that supply blood to the heart, the technology had proven difficult to adapt for brain applications owing to several technical challenges.
One major challenge is that the fiber-optic probes used in the technology are typically quite stiff, making them too rigid to twist and bend through the convoluted passageways of the brain’s vasculature. Additionally, the torque cables—traditionally used to rotate the OCT lens to image surrounding vessels and devices in three dimensions as the probe retracts—were too large to fit inside the catheters that are telescopically advanced into the brain’s arteries to address blockages or other vascular issues.
“We had to invent a new technology,” Ughi explains. “Our probe had to be very, very flexible, but also very, very small to be compatible with the clinical workflow.”
To achieve these design criteria, Ughi and his colleagues altered the properties of the glass at the heart of their fiber-optic cables, devised a new system of rotational control that does away with torque cables, miniaturized the imaging lens, and made a number of other engineering innovations.
The end result: a slender probe, about the size of a fine wire, that spins 250 times per second, snapping images as it glides back through the blood vessel. Researchers flush out blood cells with a tablespoon of liquid, then manually or automatically retract the probe, revealing a section of the artery about the length of a lip balm tube.
Neurosurgeon Vitor Mendes Pereira has grown accustomed to treating brain aneurysms with only blurry images for guidance.
Equipped with a rough picture of the labyrinthine network of arteries in the brain, he does his best to insert mesh stents or coils of platinum wire—interventions intended to promote clotting and to seal off a bulging blood vessel.
The results are not always perfect. Without a precise window into the arterial architecture at the aneurysm site, Pereira says that he and other neurovascular specialists occasionally misplace these implants, leaving patients at a heightened risk of stroke, clotting, inflammation, and life-threatening ruptures. But a new fiber-optic imaging probe offers hope for improved outcomes.
PEREIRA ET AL./SCIENCE TRANSLATIONAL MEDICINE
According to Pereira’s early clinical experience, the technology—a tiny snake-like device that winds its way through the intricate maze of brain arteries and, using spirals of light, captures high-resolution images from the inside-out—provides an unprecedented level of structural detail that enhances the ability of clinicians to troubleshoot implant placement and better manage disease complications.
“We can see a lot more information that was not accessible before,” says Pereira, director of endovascular research and innovation at St. Michael’s Hospital in Toronto. “This is, for us, an incredible step forward.”
And not just for brain aneurysms. In a report published today in Science Translational Medicine, Pereira and his colleagues describe their first-in-human experience using the platform to guide treatment for 32 people with strokes, artery hardening, and various other conditions arising from aberrant blood vessels in the brain.
Whereas before, with technologies such as CT scans, MRIs, ultrasounds, and x-rays, clinicians had a satellite-like view of the brain’s vascular network, now they have a Google Street View-like perspective, complete with in-depth views of artery walls, plaques, immune cell aggregates, implanted device positions, and more.
“The amount of detail you could get you would never ever see with any other imaging modality,” says Adnan Siddiqui, a neurosurgeon at the University at Buffalo, who was not involved in the research. “This technology holds promise to be able to really transform the way we evaluate success or failure of our procedures, as well as to diagnose complications before they occur.”
A Decade of Innovation
A four part figure showing a diagram of the probe and placement in a human brain.The new fiber-optic probe is flexible enough to snake through the body’s arteries and provide previously unavailable information to surgeons.PEREIRA ET AL./SCIENCE TRANSLATIONAL MEDICINE
The new imaging platform is the brainchild of Giovanni Ughi, a biomedical engineer at the University of Massachusetts’ Chan Medical School in Worcester. About a decade ago, he set out to adapt a technique called optical coherence tomography (OCT) for imaging inside the brain’s arteries.
OCT relies on the backscattering of near-infrared light to create cross-sectional images with micrometer-scale spatial resolution. Although OCT had long been used in clinical settings to generate pictures from the back of the eye and from inside the arteries that supply blood to the heart, the technology had proven difficult to adapt for brain applications owing to several technical challenges.
One major challenge is that the fiber-optic probes used in the technology are typically quite stiff, making them too rigid to twist and bend through the convoluted passageways of the brain’s vasculature. Additionally, the torque cables—traditionally used to rotate the OCT lens to image surrounding vessels and devices in three dimensions as the probe retracts—were too large to fit inside the catheters that are telescopically advanced into the brain’s arteries to address blockages or other vascular issues.
“We had to invent a new technology,” Ughi explains. “Our probe had to be very, very flexible, but also very, very small to be compatible with the clinical workflow.”
To achieve these design criteria, Ughi and his colleagues altered the properties of the glass at the heart of their fiber-optic cables, devised a new system of rotational control that does away with torque cables, miniaturized the imaging lens, and made a number of other engineering innovations.
The end result: a slender probe, about the size of a fine wire, that spins 250 times per second, snapping images as it glides back through the blood vessel. Researchers flush out blood cells with a tablespoon of liquid, then manually or automatically retract the probe, revealing a section of the artery about the length of a lip balm tube.
ST. MICHAEL’S FOUNDATION
Clinical Confirmation
After initial testing in rabbits, dogs, pigs, and human cadavers, Ughi’s team sent the device to two clinical groups: Pereira’s in Toronto and Pedro Lylyk’s at the Sagrada Familia Clinic in Buenos Aires, Argentina. Across the two groups, neurosurgeons treated the 32 participants in the latest study, snaking the imaging probe through the patients’ groins or wrists and into their brains.
The procedure was safe and well-tolerated across different anatomies, underlying disease conditions, and the complexity of prior interventions. Moreover, the information provided frequently led to actionable insights—in one case, prompting clinicians to prescribe anti-platelet drugs when hidden clots were discovered; in another, aiding in the proper placement of stents that were not flush against the arterial wall.
“We were successful in every single case,” Ughi says. “So, this was a huge confirmation that the technology is ready to move forward.”
“We can see a lot more information that was not accessible before.”
—VITOR MENDES PEREIRA, ST. MICHAEL’S HOSPITAL
A startup called Spryte Medical aims to do just that. According to founder and CEO David Kolstad, the company is in discussions with regulatory authorities in Europe, Japan, and the United States to determine the steps necessary to bring the imaging probe to market.
At the same time, Spryte—with Ughi as senior director of advanced development and software engineering—is working on machine learning software to automate the image analysis process, thus simplifying diagnostics and treatment planning for clinicians.
Bolstered by the latest data, cerebrovascular specialists like Siddiqui now say they are chomping at the bit to get their hands on the imaging probe once it clears regulatory approval.
“I’m really impressed,” Siddiqui says. “This is a tool that many of us who do these procedures wish they had.”
MRI Lie Detectors ›
The Superconducting Shields Behind MRIs’ Triumph ›
Elie Dolgin is a science writer specializing in biomedical research and drug discovery.

Leave a Reply