by KU Leuven
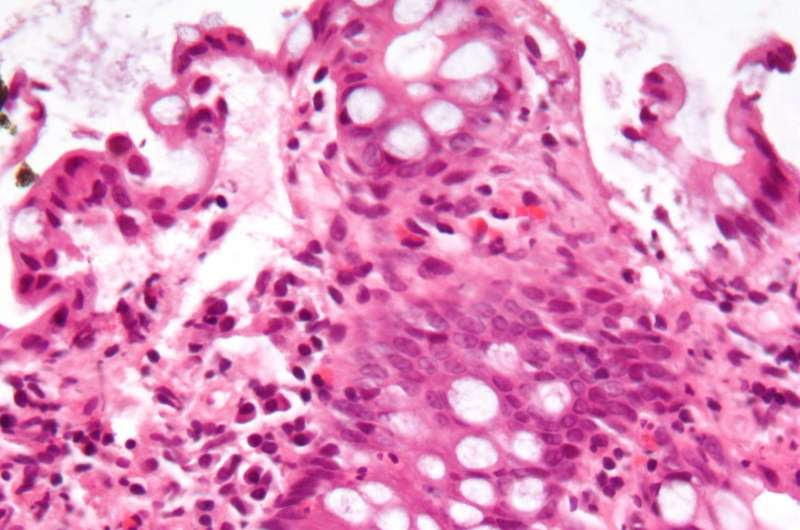
Micrograph showing inflammation of the large bowel in a case of inflammatory bowel disease. Colonic biopsy. Credit: Wikipedia/CC BY-SA 3.0
A method that instructs immune system cells to help repair damaged tissues in the intestine has been developed by researchers at KU Leuven and Seoul National University. This opens the way for more effective treatment of inflammatory bowel disease, including ulcerative colitis and Crohn’s disease. The study was carried out on humans and mice.
When functioning correctly, the immune system protects against harmful agents such as bacteria that get into the body. But in conditions such as inflammatory bowel disease (IBD), the immune system attacks the tissues that line the gut, forming ulcers and causing pain and discomfort. Nearly 3.9 million women and 3.0 million men are living with IBD worldwide, and the number of cases is rising.
Since the origin of IBD is unknown, treatments often focus on reducing the immune response in order to limit inflammation and the resulting symptoms. But this also hinders those parts of the immune system involved in repairing the damaged intestine. For example, the white blood cells known as macrophages (literally ‘big eaters’ in Greek) play a variety of roles in both inflammation and tissue repair. They consume foreign bodies, clear up debris from damaged cells, and release substances that direct other steps in the inflammatory or repair processes.
“Our idea is that the migration of macrophages to the damaged tissue in IBD is essential to stimulate its recovery,” explains Professor Gianluca Matteoli, an immunologist at the Translational Research Center for Gastrointestinal Disorders (TARGID) KU Leuven and lead author of the research, published this week in the journal Gut. His team, and that of Professor Seung Hyeok Seok from Seoul National University, set out to test this theory.
When the researchers looked at macrophages in the intestines of a handful of people with IBD, a sub-group of cells able to respond to prostaglandin E2 (PGE2) stood out. Prostaglandins are messenger molecules in the immune system, associated with tissue regeneration.
“If the patients had acute disease, they had a lower amount of these beneficial cells, and if they went into remission, then amounts of macrophages went up. This suggests that they are part of the reparative process,” Professor Matteoli says.
To investigate further, the researchers turned to a mouse model for ulcerative colitis, one of the main forms of IBD. The number of macrophages sensitive to the prostaglandin was lower in the model than in healthy mice, but if PGE2 levels were increased, the few sensitive macrophages present responded, releasing a substance that in turn stimulated tissue regeneration.
If the PGE2 receptors on the macrophages were knocked out, making them unable to respond to the prostaglandin, the level of tissue regeneration dropped. But it could be restored by getting the macrophages to swallow a liposome (a bubble of material similar to a fragment of cell wall) containing a substance able to trigger the release of the repair stimulating agent.
“We already knew that prostaglandins were important for inducing proliferation of tissue cells, but this study shows that they are also important for controlling the inflammatory effect, so moving the body from the acute stage where inflammation dominates to the reparative stage,” Professor Matteoli says.
The prospects for new treatments lie in liposomes used to jump-start the macrophages into stimulating tissue repair. The technique is well-established as an experimental tool, but applications like this are rare. “This is one of the first times it has been used to produce a beneficial, therapeutic effect,” says Professor Seok. However, a lot of work will be needed before it can be used in patients.
The next step is to look in detail at human macrophages at different stages of IBD. “We want to identify other factors that trip the switch that turns macrophages from inflammatory cells to non-inflammatory cells,” says Professor Matteoli. “Then, using the liposome technology that Professor Seok has developed, these could be used to target the macrophages and so produce very precise drugs.”

Leave a Reply